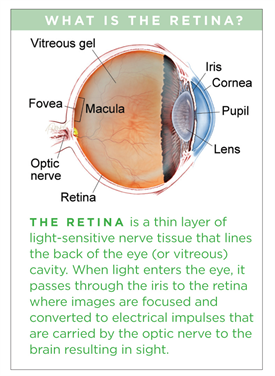
Central serous chorioretinopathy, commonly referred to as CSC, is a condition in which fluid accumulates under the retina, causing a serous (fluid-filled) detachment and vision loss.
CSC most often occurs in young and middle-aged adults. For unknown reasons, men develop this condition more commonly than women. Vision loss is usually temporary but sometimes can become chronic or recur.
 Symptoms
Symptoms
Blurry central vision, which often occurs in one eye, is the most common symptom that patients experience; however, careful examination often reveals some involvement in the other eye as well.
Depending on the location and amount of sub-retinal fluid, CSC can show no symptoms, especially if the affected areas fall outside of the macula—the part of the retina used to distinguish fine detail for activities like reading and recognizing faces.
Causes
The causes of CSC are not fully understood. It is thought that any systemic exposure to a corticosteroid drug can bring about or worsen CSC. Corticosteroids are found in allergy nose sprays and anti-inflammatory skin creams available over the counter, and are often prescribed to treat a variety of medical conditions.
An association has also been made between CSC and patients with emotional distress and/or “type A” personalities. It is possible that the body produces natural corticosteroids in times of stress that may trigger CSC in an individual prone to this condition.
Risk Factors
About half of patients diagnosed with CSC have at least one relative with findings of the disease on retinal examination. This indicates that there may be a genetic tendency; however, no specific inheritance pattern has been identified.
Patients with high blood pressure or heart disease, and those with a current or recent pregnancy have been shown to have a higher risk of developing CSC.
Beyond corticosteroids, there is evidence that other drugs including stimulants, decongestants, erectile dysfunction medications, and some anti-cancer agents may trigger CSC. Be sure to tell your doctor about any medication you are taking.
Diagnostic Testing
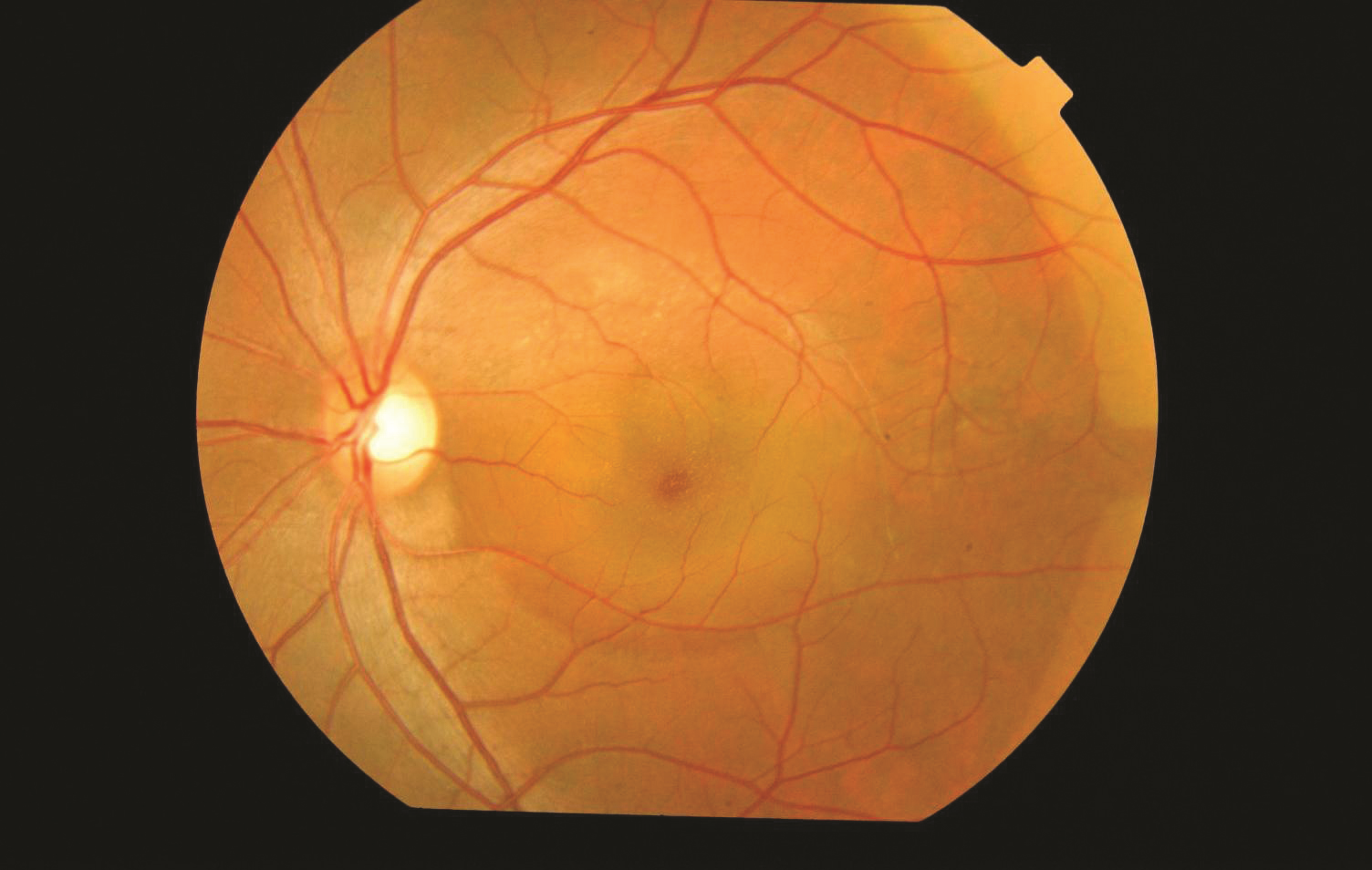
Your doctor will conduct a complete dilated eye examination in both eyes, and will obtain imaging of the retina. Retinal photographs may be taken to document the appearance of disease.
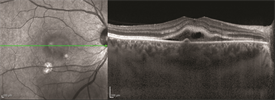
Optical coherence tomography (OCT) is a retinal scan that is very helpful in diagnosing CSC; it enables your doctor to see the retina at the microscopic level. This makes it possible to identify very small pockets of fluid or retinal scarring (once the fluid has subsided) in acute or chronic CSC (Figure 1).
Fluorescein angiography is a test in which a dye is injected into a patient’s arm vein and pictures are taken of each eye to detect characteristic leakage of the dye beneath the patient’s retina. This test, along with OCT, allows your doctor to make the diagnosis of CSC and to distinguish it from other retinal diseases causing fluid in the macula.
Treatment and Prognosis
CSC is typically a self-limiting disease, and visual recovery usually occurs within a few weeks to months without treatment.
Patients who are taking corticosteroids of any kind should discontinue their use if possible, but only after checking with their prescribing physician to ensure it is safe to stop. Suddenly discontinuing high-dose steroid medications can cause medical problems.
Several therapies have been used to treat chronic CSC, including thermal laser treatments, oral medications, and eye injections. A “cold laser,” called photodynamic therapy, is also effective and often used to focally treat the source of fluid leakage under the retina in chronic CSC.
With photodynamic therapy, a drug called verteporfin is injected into the arm, where it travels to the eye. The verteporfin is activated by shining a special cold laser on the source of leakage in chronic CSC. It may also prevent future recurrences in some eyes.
Depending on the severity and timeline of your symptoms, your doctor will choose the best treatment option, which often begins with a trial of observation. Early detection of CSC is very helpful, and most eyes with CSC can be treated successfully to avoid permanent vision loss.
Authors
Thank You To The Retina Health Series Authors
Sophie J. Bakri, MD
Audina Berrocal, MD
Antonio Capone, Jr., MD
Netan Choudhry, MD, FRCS-C
Thomas Ciulla, MD, MBA
Pravin U. Dugel, MD
Geoffrey G. Emerson, MD, PhD
Roger A. Goldberg, MD, MBA
Darin R. Goldman, MD
Dilraj S. Grewal, MD
Larry Halperin, MD
Vincent S. Hau, MD, PhD
Suber S. Huang, MD, MBA
Mark S. Humayun, MD, PhD
Peter K. Kaiser, MD
M. Ali Khan, MD
Anat Loewenstein, MD
Mathew J. MacCumber, MD, PhD
Maya Maloney, MD
Hossein Nazari, MD
Oded Ohana, MD, MBA
George Parlitsis, MD
Jonathan L. Prenner, MD
Gilad Rabina, MD
Carl D. Regillo, MD, FACS
Andrew P. Schachat, MD
Michael Seider, MD
Eduardo Uchiyama, MD
Allen Z. Verne, MD
Yoshihiro Yonekawa, MD
Editor
John T. Thompson, MD
Medical Illustrator
Tim Hengst
Downloads
Copyright 2016 The Foundation of the American Society of Retina Specialists. All rights reserved.